… Continued …
Blood sugar level monitoring
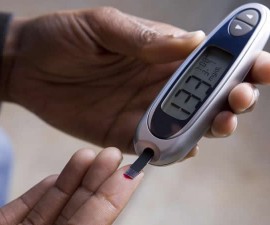
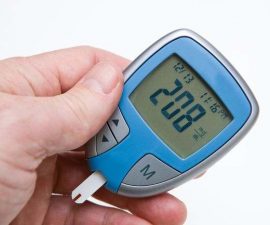
Since diabetes can make your blood sugar fluctuate easily, test your blood sugar regularly! You can do it at home with portable glucose meter, a practical device that measures the level of your blood sugar in a small drop of blood.
When to take the test? This can vary from person to person. But in general, you may need to take it twice a day or more if you take insulin. It’s usually recommended to do it before meals and if necessary before your bedtime.
But if you’re not taking insulin or only use lifestyle measures to control your type-2 diabetes, you may not need to take the test daily. See also the normal blood sugar targets for diabetics in here!
In addition, your doctor may suggest HbA1c test at least once a year. It is used to show how well your blood sugar is managed over the long term. This also can help analyze the effectiveness of the treatment or lifestyle measures you follow to cope with the disease.
Healthy-balanced diet
What you eat can affect your blood sugar, especially true for high-GI foods. GI or glycemic index is a variable used to determine how fast a food in affecting blood sugar. Low-GI foods are more recommended for diabetics since they are slowly digested (you can feel full longer), and the most important thing they have least effect on blood sugar.
On the other hand, high-GI foods can quickly affect your blood sugar level. They are quickly digested and absorbed in the body. Learn more about healthy-balanced diet, foods to eat and avoid for people with diabetes in this section!
Limit alcohol and avoid smoke!
Alcohol can cause too high or too low blood sugar. This is dependent on the amount you drink. It may also affect some diabetes treatment. For instance, sometimes it can affect your ability to carry out insulin treatment. So be careful when drinking, do it only in moderation or avoid it (especially true when your stomach is empty, never drink with empty stomach)!
Tobacco smoke is also bad for diabetics. It can increase the risk of diabetic complications such as stroke and heart disease. Even it is very bad for non-diabetics, too! So like a well-known adage, say ‘NO’ for smoking!
Keep active, regular exercise!
Diabetes is often associated with lack of energy and weakness, even though if you have eaten. This is because the body cannot effectively use glucose for energy.
However, this doesn’t mean you can forget your exercise! Instead, regular exercise is so essential to help control blood sugar in diabetics, improve your overall fitness, and decrease the risk of diabetic complications (especially such as cardiovascular diseases). For non-diabetics, exercise can help improve insulin sensitivity and lower the risk of type 2 diabetes.
But exercise when you have diabetes also poses unique challenges. This is particularly true if you take insulin to help control the disease. There may be particular instructions you need to follow to exercise safely.
For example, it’s usually recommended to test your blood sugar before exercise and make sure it’s at least 100 mg/dL if you take insulin. And like anyone else, take at least 2 hours and 30 minutes a week of moderately intense workouts such as fast walking, swimming, or bicycling. Talk to your doctor or care team for more advice!
Good relationship with others
Stress, depression, and anxiety are quite common in people with chronic condition. As mentioned before, diabetes requires consistency, persistence, and hard work to manage. Not all patients can cope with it successfully. Sometimes it may also carry relationship problem with others, making everything more difficult.
Many diabetics find that it’s helpful to talk with others in a similar position. Find a group of people with diabetes in your local area, and join with them! You can share what you think and your experience. Build a good relationship with others!
Don’t forget to make a regular contact with your care team, since type 2 diabetes is a long-term medical condition. Having a good relationship with your diabetes care team will enable you to keep monitoring the disease better.
- https://www.nlm.nih.gov/medlineplus/ency/article/000313.htm
- Oct. 29, 2015, New England Journal of Medicine